The Importance of WHO’s SMART Guidelines In Public Health Implementations by Kunjan Patel on June 28, 2022 3,681 views

The ongoing COVID-19 pandemic has brought renewed focus on public health. A push for rapid digitization of existing public health infrastructure, patient health data management and interoperability were some of the effects of this pandemic by way of response. With rapid digitization, especially developing countries started to experience teething troubles and have poor data policies. As the world moves toward a digital health future, inconsistency and lack of proper guidelines and recommendations are the biggest hurdles in the current scenario.
As the specialized United Nations agency responsible for international public health, WHO issues public health policies, guidelines and clinical data recommendations. These are pivotal for countries in architecting meaningful health interventions and evidence-based practices to improve the overall health of the population at large.
SMART guidelines, a meaningfully thought-out acronym for Standards-based, Machine-readable, Adaptive, Requirements-based, and Testable, play a significant role in ensuring that WHO guidelines are translated accurately on ground zero. The ground zero here is the level where the HCWs (Health Care Workers) carry out the daily tasks such as screening, classifying and assessing, and much more, for taking care of the targeted population they have been assigned leveraging digital tools like mobile phones.
Communication loss is the biggest challenge that results in the dilution of WHO’s guidelines at various levels. Ultimately, this results in watered out/inferior quality/completely wrong public health implementations in localized contexts. In simple terms, consider these guidelines an effective vaccine against the Chinese whispers prevailing across public health systems trying to implement WHO’s health policies, guidelines and clinical data recommendations.
This blog will attempt to cover SMART Guidelines in detail and explain some of the Public Health concepts necessary to understand the blog while also underscoring the pivotal role they play in ensuring that grand public healthcare goals are achieved with utmost practicality on ground zero.
WHAT IS PUBLIC HEALTH & HOW IS IT DIFFERENT FROM CLINICAL HEALTH?
Public health is related to taking care of a larger swath of the population. It is the science of protecting the health of a large community or as small as individuals. While doctors treat us when we are already sick, public health professionals try to prevent us from being sick in the first place. A classic example is that public health professionals would try to prevent the spread of COVID-19 by promoting regular hand washing, maintaining social distancing and wearing masks. In contrast, a clinical health professional would work on an individual after being infected with the COVID-19 virus.

WHAT ARE SMART GUIDELINES?
SMART Guidelines were envisioned as a set of comprehensive digital health implementation guidelines. These guidelines were devised as a five-step pathway (Layer 1 to Layer 5, explained below) – which, if adhered to – will fast-track the adoption of the best clinical and public health data practices. As the adoption rate for digital health systems increases and countries invest in digital technologies to meet public healthcare challenges, SMART guidelines provide invaluable support to the implementing countries.
WHY ARE SMART GUIDELINES NECESSARY?
A larger measure of the success of digital health interventions in-country context is the accuracy of interpretation of WHO’s recommendations and adaptation of content complying with policies, procedures and digital tools. However, ‘the devil,’ as they say, ‘lies in the details.’ Bird’s eye view-level observations have historically revealed that the process of implementing WHO recommendations at the country level leaves many gaps. Moreover, the process has been slow-paced, unsystematic, and prone to errors. And it has been plagued by a lack of compliance with internationally agreed-upon technical standards.
Quite often, the lack of guidance concerning the technology and health content has rendered less-than-perfect digital solutions. This has repercussions in the form of a lack of confidence and, therefore, investments. Furthermore, due to hard-coding quite often, digital solutions cannot be agile to evolving content alignment as the health evidence evolves. Further, badly envisioned digital solutions offer poor interoperability options and country-based localization due to the rigidity written into solutions. Ultimately, the gains supposed to accrue to the targeted beneficiaries due to digital health solutions suffer.
Against this backdrop, SMART guidelines help plug gaps and support WHO’s vision of a future where people everywhere benefit from its health and data recommendations. The next part of the content digs deeper into the various layers (L1 to L5) of the SMART guidelines and tries to make it simple to understand the concept.
Digging deeper into SMART Guidelines
Any digital health software solution across the globe would have the below-mentioned aspects:
- Envisioned top-level functional requirements (here, L1)
- Functional documentation covering the top-level requirements (here, L2)
- Technical documentation translated from the functional requirements (here, L3)
- The actual functional application – Web, Mobile App, or Standalone (here, L4)
- Peripheral functional & non-functional analytics (here, L5).
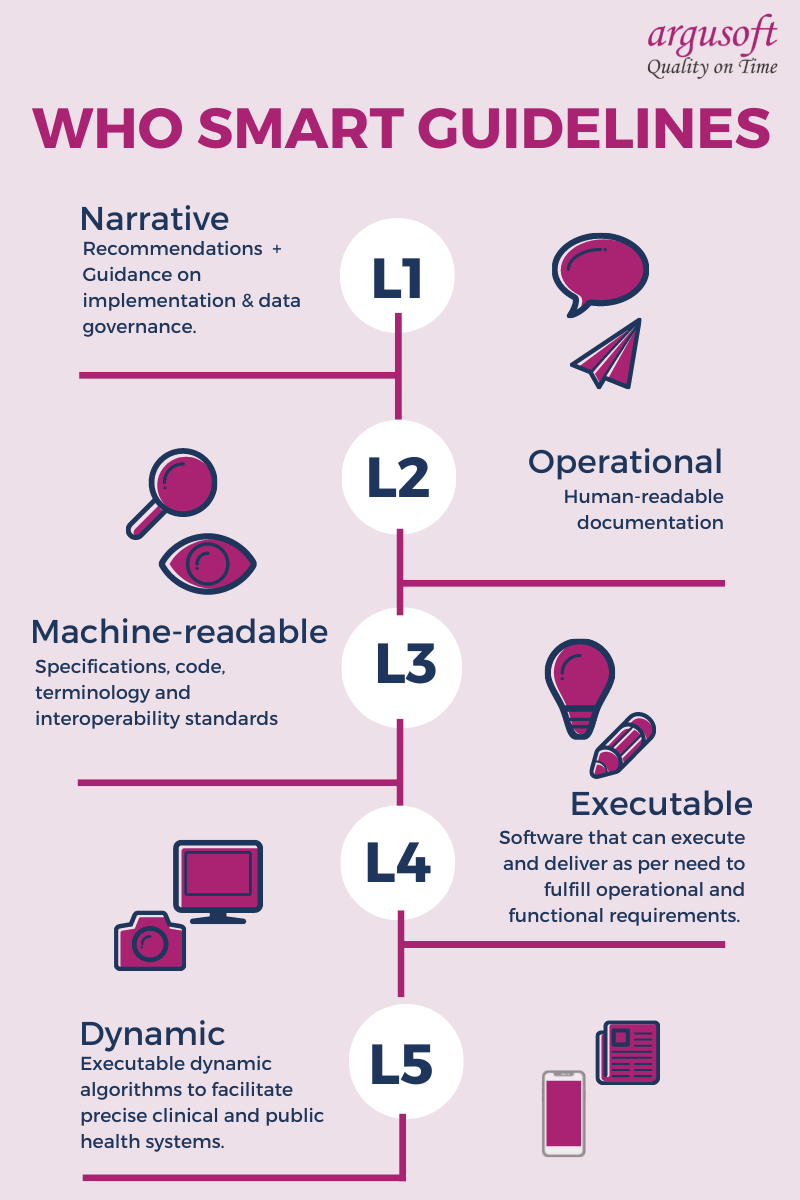
Now, let’s dig deeper into each of the layers – keep in mind the level coding attached to each of the points above for better understanding.
SMART Guidelines Layers
L1: Narrative Layer
L1 is the first knowledge layer. This layer consists of traditional guidelines and guidance. It details ideas to streamline the current guideline development process to support digital transformation. L1 elaborates on the need for registering and uniquely identifying recommendations. These recommendations are updated promptly to make sure the context remains contemporary. It is done based on the evidence collected, which improves with time. This layer may be considered akin to the origin story of digital solutions.
L2: Operational Layer
L2 or the operational layer delves into the requirements base and starts documenting the L1 knowledge layer. This documentation is software-neutral and human-readable. Elements such as recommendations, personas, user scenarios, decision support logic, algorithms, data sets, workflows, business processes etc., are penned down and compiled into a Digital Adaptation Kit (commonly known as a DAK). Consequently, the operationalization becomes consistent, and transparency is built into it.
L3: Machine-readable Layer
The third layer aims to deliver a structured set of software-neutral ” machine-readable specifications. This means that these specifications can be imported into a digital reference software that understands them and renders them meaningfully to create system workflows intended by the guidelines. These specifications adhere to the highest interoperability standards and are covered by technical and medical terminologies such as ICD and SNOMED. In addition, the specifications conform with the HL7® FHIR® (Fast Healthcare Interoperability Resources) standards.
To contextualize this better, the FHIR specifications define how healthcare information is exchanged between different computer systems. These guidelines allow the need-based access to and availability of healthcare information (clinical and administrative data). Ultimately, this benefits patients due to an increase in transparency and consistency. In addition, Digital Solutions that accommodate L3 recommendations can be tested for compliance with interoperability standards.
L4: Executable Layer
The fourth layer is the actual reference software that understands the L3 specifications and creates meaningful workflows. This software translates the specifications to deliver the operational and functional requirements.
The fully functional software works as a starting point – which can be readily localized to suit diverse operational contexts for various countries and geographical areas. Moreover, given that the layer uses specifications mentioned in the L3, the data representation is consistent everywhere. This aids the interoperability of the software. Moreover, there are a lot of open-source software libraries that can be used to build reference software. One such example is Google’s upcoming FHIR SDK (available in the BETA version) which enables the creation of Android applications easily by providing useful APIs. Another example is the HAPI FHIR Library available for JAVA-based applications.
L5: Dynamic-precision health models
The final knowledge layer uses big data, dynamic algorithms, and advanced analytics to achieve desired outcomes. The L4 digital systems, when implemented and scaled up, facilitate the creation of country-specific, anonymized, globally collected, and normalized data. Further, with the application of AI and Machine Learning, context specificity is achieved. The algorithms are optimized for a given population and its desired health outcomes.
Argusoft – Your Digital Transformation Enabler
Under our close multidimensional collaboration with WHO, we have had exposure to SMART guidelines. In addition, we are working in tandem with WHO to develop and implement the EmCare reference software – an L4 app. The app offers clinical decision support to frontline health workers in emergency settings in line with WHO recommendations. The project’s inception happened around a year ago, in September 2021. Currently, the project is in the development stage. We are actively working with the stakeholders and content creators of the L2 and L3 layers to build a robust framework that can accommodate the SMART Guidelines and is configurable for the most part. The reference software has an Android-based application built with the help of Google’s FHIR SDK that has supported FHIR specifications-related aspects. Additionally, we are also contributing to the same SDK’s development along with the wider community.
The project is planned to be piloted in a couple of countries in September 2022 with a pre-decided limited number of features. A more detailed and enhanced software shall be rolled out after the pilot’s feedback and detailed case studies.
Moreover, the SMART guidelines have received a good response from the stakeholders and community worldwide. WHO has been actively working on engaging the community regularly and has created many platforms for exchanging information regarding things happening in the SMART Guidelines direction.
We understand that the systemic change in country-specific public healthcare outreach is often complex and comprehensive. This is where WHO’s SMART guidelines have a pivotal, reconciliatory, and somewhat regulatory role. Therefore, we will continue to support WHO as it takes upon itself the mammoth tasks of digital health system transformation and achievement of universal health coverage and UN Sustainable Development Goals.
Argusoft specializes in creating elegant digital solutions for the health tech space with a special focus on public health initiatives in under-serviced regions worldwide. Our long-standing association with the WHO in several projects deserves special mention. Moreover, Argusoft’s proprietary health tech solution ‘MEDPlat’ is now one of India’s first 40 digital health solutions to be successfully integrated with the government’s Ayushman Bharat Digital Mission (ABDM).
We look forward to contributing deeply to the intersection of technology and public health in the coming years. SMART guidelines will play a pivotal role in this space, and we are glad to have the opportunity to contribute to it.